Department of Health and Human Resources
Children's Health Insurance Program
(CHIP)
SPECIAL REPORT
The West Virginia Children's Health Insurance Program (CHIP) has been in existence for nearly two years. It was established within the Department of Health and Human Resources (DHHR) in the 1998 Legislative session in response to federal legislation. The first board meeting took place in June 1998. It was decided by the Legislature that the first phase (CHIP I) of the program for children between the ages of 1 and 5 would be a Medicaid expansion. Since Medicaid was administered through the Recipient Automated Data Information System (RAPIDS), this computer system was also used to determine CHIP eligibility. In retrospect, this was a logical decision according to the CHIP Board Chairman and its Executive Director, because it allowed the CHIP program to provide health coverage for uninsured, low-income children as soon as possible. It also allowed CHIP to avoid duplicating functions available in existing agencies, which was a requirement of the State mandate.
The implementation of CHIP I was relatively smooth with some exceptions. There were 24 children enrolled in CHIP I as of July 1, 1998. This figure has increased to over 1,200 (see Table 1). However, implementing the second phase (CHIP II) for children between the ages of 6 and 18 encountered difficulties stemming from communication breakdowns between DHHR and the CHIP Policy Board. The number of children in CHIP II has surpassed 8,000.
TABLE 1
Children Enrolled in CHIP as of January 31, 2000
| CHIP I | CHIP II |
| 1,206 | 8,484 |
The purpose of this section is to provide a backdrop for why the CHIP program was removed from DHHR during this past legislative session, which is explained in Issue 1.
The Board Considers 12 Month Continuous Coverage Essential for CHIP
The primary problem focused on a decision made by the Board that it wanted eligible children to have 12 months continuous health insurance coverage. Once children were determined eligible for the CHIP program, the Board did not want them to lose coverage during the 12 month period. For example, if income increased making them ineligible for CHIP, or if income decreased making them eligible for Medicaid, the Board wanted the children to remain in the CHIP program. Prior to the end of the 12 month period, clients would be redetermined for another 12 month period, at which time they would be removed from the program if they were no longer eligible.
The Board was adamant on this point and it was clearly indicated to DHHR from the beginning. Delegate Leach, ex-officio member of the Board, advised the Board that the intent of the Legislature was to create a health program that would establish eligibility on an annual basis, not a month-to-month basis. Senator Walker, another ex-officio member, concurred, noting that the expenses to mail out eligibility redetermination information on a monthly basis would be better spent on health costs. Senator Walker stated that she thought it would be a good idea to have a 12 month continuous eligibility period. In August of 1998, the Board officially decided that CHIP II eligibility would be continuous for a 12 month period regardless of any change in income, and that for children in CHIP I continuous eligibility would also be implemented.
4 Months Later the Board Realizes that 12 Months Continuous Coverage Would Not be Implemented Exactly as Specified
Despite the Board's clearly stated intent for the program, modifications to the RAPIDS system for 12 month continuous coverage were not exactly as the Board specified. The modifications were successful in keeping children on CHIP for 12 months even if their family's income increased to where they are ineligible for CHIP. However, when family income decreased to where the children become eligible for Medicaid, children are automatically taken off of CHIP and placed on Medicaid. This exception was unacceptable to the Board, and the Board felt that it was not adequately informed by DHHR of this important exception.
The Change Order for these modifications was valued at $434,855 and it was drafted about one month after the Board made its final decision on 12 month continuous coverage. According to DHHR, after the Change Order was drafted, DHHR informed the Board's staff on numerous occasions that federal regulations and state policy prohibited 12 months continuous eligibility if children became Medicaid eligible during the 12 month period. However, it was 4 months after the Change Order was drafted that the Board clearly understood that the modifications could not be made exactly as specified by the Board. Furthermore, the Board was informed by DHHR that the modifications desired by the Board would result in additional costs totaling nearly $1 million dollars. At issue is whether the contract to perform the modifications was specified to comply with the Board's intent, but that the changes were found to be more complicated and costly than originally estimated. This leads to the question of whether the Board paid for services not rendered.
Deloitte and Touche, the contracted vendor responsible for modifying the RAPIDS system, indicates that its original Change Order in September of 1998, which was reviewed by DHHR, did not intend to provide 12 month continuous coverage as specified by the Board. In cases where a child becomes Medicaid eligible within the 12 month period, the child would have to be taken off of CHIP and placed on Medicaid. The vendor contends that:
We continually pointed out that although we could "skip" the income check in the CHIP eligibility determination when a CHIP eligible had an increase in income (e.g., increasing their income to a level of more than 150% of the Federal Poverty Level), the DHHR is unable, by court order, state policy and federal statute, to bypass giving a client a more comprehensive Medicaid coverage than CHIP, when the CHIP eligible experiences a decrease in income... (emphasis included)
DHHR also contends that federal regulations and state policy prohibited keeping children on CHIP if income dropped during the 12 month period to where they become Medicaid eligible. Therefore, their argument is that the Change Order was never specified to provide 12 month continuous coverage the way the Board intended, because it was prohibited by federal regulations and state policy.
Documentation provided to the Legislative Auditor's Office does not allow determination if the Board paid for services not rendered because the Change Order stated that the cost estimate was subject to change because some decisions had not been finalized by the Board at the time it was drafted. It is also not clear if the Change Order was originally specified to meet the Board's original intent. The Change Order did not have clear specifications as to what it would do. The language is brief and technical, and there is no overall description of how the programming would work under certain scenarios. There is one clear statement in the Change Order under a non-financial test for eligibility which states:
once determined eligible, the individual remains eligible for a predetermined time period regardless of any change in income.
This language suggests that a client would remain in CHIP II even if income increased or decreased. However, given the lack of clear definition of the Change Order, it is not certain how this above statement fit in with the overall programming. Furthermore, DHHR's RAPIDS staff indicated that it was responsible to determine what the Board wanted and then instruct Deloitte and Touche on what changes were to be made. With this understanding, Deloitte and Touche was contracted to do only what DHHR staff instructed it to do.
What is clear is that this problem resulted from a lack of clear and timely communication, either from DHHR to the Board's staff, or from the Board's staff to the Board members. This is shown by the following:
The Legislative Auditor concludes that DHHR was slow in attempting to obtain written clarification from HCFA concerning whether federal regulations would allow the Board's design to be implemented, and HCFA contributed to the problem by its indecisiveness and conflicting statements. The fact that DHHR was seeking clarification as late as January of 1999 indicates it did not understand if regulations prohibited the Board's intent. Written clarification should have been sought from HCFA as early as August of 1998. The first documented attempt at clarification was made in January of 1999 and written clarification was obtained January of 2000. Ironically, the Board now realizes that its original intent could have been accomplished under federal regulations. However, early confusion concerning HCFA policy precluded the program from achieving an important element the Board wanted.
Agitated Board Reluctantly Compromises on 12 Month Continuous Coverage
An emergency meeting of the CHIP Board was held on January 15, 1999 to discuss the inability to have modifications made to the RAPIDS system comply with the Board's original intent. The chairman of this meeting stated:
The Board is very disturbed to only recently learn that the RAPIDS system cannot perform the 12 month continuous eligibility without delaying the start of Phase II and requiring a significant cost of $1,000,000.
After a lengthy discussion, the Board accepted the changes discussed to the program's 12 month continuous eligibility, which meant that children would be in CHIP II for 12 months except when income dropped and they became Medicaid eligible during the 12 month period. In this case, the RAPIDS system would automatically remove the child from CHIP II and place the child on Medicaid.
CHIP Program Operates with Fewer Problems, but not as Envisioned
Currently, the CHIP program works with few problems, although it is not as the Board originally envisioned. Without 12 month continuous coverage as originally planned, the program lacks the continuity the Board wanted, and it experiences administrative confusion. Many cases are routinely closed before 12 months for reasons such as moving out of state, or turning 19 years of age. These types of closures are unavoidable and acceptable. However, most closures are due to families becoming eligible for Medicaid. Table 2 shows the number of closures that occurred between September 1, 1999 and January 31, 2000. On average, nearly 7% of the caseload experienced closures each month. RAPIDS staff estimated that 67% of closures were due to children becoming Medicaid eligible. This particular type of closure was not what the Board wanted. Although it is a benefit to recipients that they are placed on Medicaid, which provides for greater coverage than CHIP, the administrative problems significantly detract from the program. For example, recipients that become Medicaid eligible will have two cards, and the health care provider does not know which card to accept or bill. It also creates some problems in determining which fund (Medicaid or CHIP) is to pay for medical treatment received during the transition period when the recipient is removed from CHIP and placed on Medicaid. (1) Although the RAPIDS system is designed to notify recipients that CHIP coverage is terminated and Medicaid coverage is effective, complaints from recipients have been received indicating they were not notified. Consequently, some recipients have been unaware that their CHIP benefits were terminated when they went for medical treatment. (2)
TABLE 2
Total Case Closures from the CHIP Program
Between September 1, 1999 through January 31, 2000
| CHIP I
Closures (1 - 5 Years of Age) |
Average Monthly Percent of Total Eligible Children | CHIP II
Closures (6 - 18 Years of Age) |
Average Monthly Percent of Total Eligible Children |
| 353 | 7.1% | 2,175 | 6.2% |
With the exception of continuous coverage, the modifications to the RAPIDS system were successful. Prior to these modifications, problems existed because CHIP applications had to be entered into RAPIDS manually. Since RAPIDS was originally designed for income parameters at Medicaid levels, RAPIDS would automatically deny CHIP applications because the income levels were above Medicaid levels. A procedure was developed, called a "work-around", that allowed workers to "override" the RAPIDS system and force it to accept CHIP applications. Work-arounds did not work smoothly for CHIP II cases. At first, CHIP II enrollees were being closed after one month. The RAPIDS system automatically reevaluated cases any time new information was entered regarding the CHIP II family, such as verification for another type of benefit eligibility, upon which RAPIDS automatically closed the CHIP II eligibility. Suddenly, a large number of children, who were supposed to have one year of medical coverage, were closed after one month. According to workers, work-arounds are no longer needed because of the modifications, and the problems associated work-arounds are resolved.
Conclusion
Continuous health insurance for 12 months, regardless of changes in income, was a critical element the Board wanted. Evidence suggests that it was four months after the Change Order was drafted that the Board clearly understood that continuous coverage could not be accomplished when children became Medicaid eligible. This required the Board to compromise on the way the program functions from the way the Board originally envisioned. Adding to the frustration is that DHHR indicated to the Board that federal regulations prohibited the Board's original program design. Now it has been clarified that federal regulations do not prohibit the original concept. The Board continues to pursue 12 month continuous coverage, however, it will do so from within the Department of Administration as Issue 1 explains. This confusion resulted from a delay by DHHR in obtaining written clarification from HCFA, and either DHHR did not clearly inform the Board's staff or the Board's staff did not understand and clearly inform Board members.
Overall, the modifications specified by RAPIDS staff and carried out by Deloitte and Touche were successful. DHHR workers indicate that initial problems with storing CHIP applications and clients being inadvertently denied coverage have been resolved since the modifications. Communication problems would have been avoided if the specifications of the Change Order were well defined and had clear examples of what the modifications would accomplish. This in turn would have allowed the CHIP Board to know immediately if the modifications were consistent with the Board's needs.
Issue Area 1: The Realignment of the Children's Health Insurance Program from DHHR to the Department of Administration Creates Important Policy Decisions.
New Legislation Sets The Scene For CHIP Changes
The Board initiated legislation to remove itself from DHHR. On March 11, 2000 legislation was passed during the regular legislative session. This legislation moved the Children's Health Insurance Program from DHHR to the Department of Administration and created the Children's Health Insurance Agency to administer the program. It also expanded the availability of medical insurance to children in families at 200% of FPL. The Board sought removal from DHHR because of strained communication, concerns over costs for work done by DHHR staff, and the strong desire to remove the CHIP program from an association with DHHR assistance programs.
The Board Faces Crucial Decisions
It is likely that by default, the removal of CHIP from DHHR could force the CHIP Board to develop a "stand-alone" computer system. However, the Board could reach an agreement with DHHR to continue the use of the RAPIDS system for eligibility purposes, but this would make the departure from DHHR serve little purpose.
There are advantages and disadvantages to a completely stand-alone computer system to determine CHIP eligibility. However, it appears that the disadvantages will outweigh the advantages if the stand-alone system has no connection with the RAPIDS system, and there is no cooperative agreement between DHHR and the CHIP Policy board. The purpose of this issue is to examine the impact of a stand-alone system.
The Advantages And Disadvantages Of A Stand-Alone Computer System
In early March of this year, a Board subcommittee considered two computer system proposals. These cost proposals are illustrated in Table 3. The first was from Deloitte and Touche to further modify RAPIDS in order to create 12 month continuous eligibility as the Board originally intended, that is, maintain clients on CHIP for 12 months even when income decreases to where they are eligible for Medicaid. Deloitte and Touche provided a cost estimate of $146,198 for 12 month continuous coverage. Deloitte and Touche also indicated costs for modifying RAPIDS to determine eligibility with expanded Federal Poverty Levels, since the Board wanted to expand to 200% FPL. The cost estimate for this feature was $569,390. To complete both functions, the cost would be $618,582.
The second proposal was made by the Information Services and Communications Technology Resource Center (IS&C) of the Department of Administration. IS&C proposed a stand-alone system to replace the current CHIP application presently residing in DHHR's RAPIDS system. The stand-alone system would be used by CHIP personnel instead of DHHR staff to determine CHIP eligibility. IS&C's proposal would provide workstations and training for CHIP personnel and an interface (connection) with the Public Employees Insurance Agency (PEIA). No interface with RAPIDS was included. The system would also eliminate the problem the Board had with the current RAPIDS system, that is the lack of 12 month continuous coverage. The total of the proposal was $70,400.
Table 3
Deloitte & Touche Cost Estimates
RAPIDS
| 12 Month Eligibility Only | Expand Income Limits W/Out 12 Month Eligibility | Expand Income Limits With 12 Month Eligibility |
| $146,198 | $569,390 | $618,582 |
Table 4
| Application | Application, Workstations | Application & Data Warehouse | Application, Workstations & Data Warehouse |
| $46,400 | $55,900 | $60,900 | $70,400 |
Advantages of A Stand-Alone System
The concept of a "stand-alone" computer system appears to solve all of the CHIP program problems.
Disadvantages
However, breaking away from the RAPIDS system is not without consequence:
Without an Integrated System, Significant "Slippage" Could Occur
A significant benefit of the current RAPIDS system is that both the CHIP program and DHHR assistance programs are in the same system. This means that when applicants apply for a DHHR program but they are eligible for CHIP, or if they apply for CHIP but they are only eligible for a DHHR program, they will be enrolled in the eligible program immediately, without any delays from having to submit a separate application for the other program.
However, in a stand-alone system that is not linked with the RAPIDS system, individuals that apply for CHIP who are ineligible but are eligible for Medicaid will have to file a separate application with DHHR. Conversely, any individual who applies for a DHHR program and is determined ineligible but is eligible for CHIP will have to submit a separate CHIP application. This could result in some individuals going some length of time, or completely, without health insurance, especially if both agencies do not adequately inform applicants of their potential eligibility for programs administered by either agency. This "slippage" could be significant if there is no cooperative agreement between DHHR and CHIP.
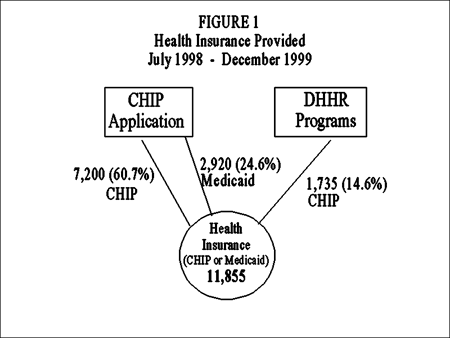
The magnitude of this potential slippage is shown in Figure 1. Between July of 1998 through December of 1999, 11,855 West Virginia children received either CHIP or Medicaid health insurance through the CHIP initiative. Of this number, 7,200 applied directly using the CHIP application and were found eligible for CHIP. However, 1,735 CHIP recipients did not actually apply to the CHIP program. Their parents applied to DHHR seeking public assistance of another sort, possibly Food Stamps, and they were found to be eligible for the CHIP program. These children were immediately enrolled in CHIP entirely due to the RAPIDS integrated computer system. Conversely, 2,920 children applied for CHIP but were not eligible because their income was too low, but they were eligible for Medicaid instead. They were immediately placed on Medicaid, and began receiving health benefits due to the RAPIDS integrated system.

If the CHIP program goes to a stand-alone computer system, it will lose an important design feature of an integrated computer system (RAPIDS) that has allowed DHHR to instantly provide health insurance to those who are either eligible for CHIP or Medicaid. Unless a method is found to link the stand-alone system to the RAPIDS system, there will be slippage for DHHR applicants eligible for CHIP, and CHIP applicants eligible for Medicaid. This will not only cause a delay in health insurance coverage, and require a second application for persons in these categories, but it may also mean that some children "fall through the cracks" and remain uncovered because the agencies do not exchange this information as an application for their program, applicants do not make the effort to file a second application, or applicants are not informed by either agency that they are eligible for another health insurance.
Conclusion
There are over 15,000 children in the State of West Virginia who have received health insurance due to the initiative of the CHIP program (See Table 5). A significant number of these children are receiving health benefits due to CHIP and Medicaid being combined in the integrated design of the RAPIDS system. Removing CHIP from DHHR, to a stand-alone system raises the "safety net" issue of children uncovered. At the end of December, 1999:
| CHIP Phase I 351 | CHIP Phase I 1,086 | CHIP Phase I 1,278 |
| CHIP Phase II 7,849 | CHIP Phase II 9,677 | |
| Medicaid 309 | Medicaid 2,920 | Medicaid 4,267 |
| TOTAL: 660 | TOTAL: 11,855 | TOTAL: 15,222 |
Today the CHIP program is poised on a new threshold due to changes in state legislation. It has achieved its goal of separating from DHHR. CHIP will move forward as a unified program, and the problems and confusion of two separate programs (CHIP I & II) will cease to exist. Clarification of the Medicaid policy enables the program to have more continuity, with CHIP recipients enrolled for a 12 month continuous period, and only an annual review for redetermination of eligibility. The Board faces a difficult decision about whether to continue to use the existing RAPIDS system, or to develop a strictly stand-alone system. It also is important for DHHR and the CHIP agency to develop a cooperative agreement to eliminate any slippage that could occur from separating CHIP eligibility functions out of the RAPIDS system. The Board should weigh the advantages and disadvantages of each approach before making a decision which will impact the future of this program and the well-being of the State's children.
Recommendation 1:
If the Children's Health Insurance Agency located within the Department of Administration should decide to develop a stand-alone eligibility computer system, then a cooperative agreement with the Department of Health and Human Resources should be developed whereby information can be exchanged between the two systems to prevent Medicaid eligible children identified by application to CHIP from going any significant length of time without health insurance. The same process should be established for children identified through the RAPIDS system as eligible for CHIP.
1. There were 431 cases in which reconciliation was needed to determine which fund was to be billed.
2. Some of the problems mentioned above are complaints made by recipients to the CHIP staff. It may be
that some recipients sought medical treatment during the time notification was in the mail. Therefore, they would
not have known they had Medicaid instead of CHIP, nor would they have even received a Medicaid card.