STATE OF WEST VIRGINIA
PRELIMINARY PERFORMANCE REVIEW OF THE
PUBLIC EMPLOYEES INSURANCE AGENCY
Contract Administration Procedures
Unclear, Reactive and Need Improvement
Issue Area 1: Contract Administration Procedures Unclear, Reactive and
Need Improvement.
A primary outcome for the PEIA is to provide health insurance to eligible individuals with the objective of achieving high customer and provider satisfaction, and administrative efficiency. The PEIA out-sources many crucial functions of the agency to private vendors through legal contracts. Since most of the functions associated with providing health insurance are carried out by private contractors, the PEIA must provide adequate oversight of the performance of its contractors to achieve the desired outcome. The finding of this review is that although there is evidence that the PEIA monitors its contracts, in some respects the oversight is reactionary, undocumented, and unclear. The effect of this is that a reactionary approach allows poor performance to exist for relatively long periods of time. Undocumented oversight presents problems in resolving disputes with vendors which could become a more serious problem if the dispute goes to court. Unclear oversight creates a problem for the agency when an individual is absent or leaves the agency and the employees' responsibilities cannot be easily assumed by someone else.
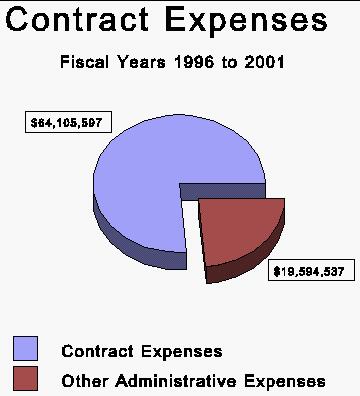
Over the past five and a half fiscal years, the PEIA has spent $64 million for professional and contractual services. This amount represents 77% of administrative expenses over this time (see Figure 1). In fiscal year 2000 for example, the PEIA reported $14.5 million in administrative and other operating expenses with contractual and professional payments representing $12.5 million of this amount. This calculation does not include claim expenses or pass through expenses for healthcare management organizations and life insurance premiums. This accentuates the importance of proper contract language, administration and oversight of vendor performance.

Overview of PEIA's Contract Administration
Based on our review, the contracts appear to be the only written document by which the
PEIA employees have guidance in monitoring contracts and vendor performance. This is
expected since the contracts drive what standards the vendor must adhere to and the
expectations of all parties involved. However, these contracts are sometimes voluminous,
full of legal jargon, and involve complicated calculations. The Legislative Auditor found
there to be few individuals within the agency delegated to vendor performance monitoring
and contract compliance assurance. There are only three individuals who are specifically
assigned to contract administration of the four contracts reviewed. The task of contract
administration is made more difficult because they also have other duties. They handle
tasks that range from plan development to customer service. For example, the person
assigned to monitoring the Claims Administration contract is also responsible for customer
service for claims, the Retiree Premium Assistance program, and Life Insurance. The person
assigned to monitoring the Pharmacy Benefits contract is also responsible for answering
correspondence concerning prescription drugs and benefits, customer service for drug
benefits, attend fairs and hearings, and act as a liaison between PEIA and contractors.
Our review noted evidence of the results of contract monitoring. Such evidence included the following:
However, in some cases it is unclear the method in which these results were
accomplished and some supporting documentation was not available. Furthermore, in some
cases the deficient performance of a vendor can be impacted by its predecessor, or the
performance of another vendor for which it receives data. The result is that PEIA's claims
of deficient performance can and have been disputed. Concern also lies in whether these
results were from diligent contract administration or after the fact customer complaints
of the contractor's performance. The latter is in the Legislative Auditor's opinion
unacceptable. Table 1 below summarizes main concerns regarding contract administration
within PEIA. We noted customer service satisfaction surveys were a part of one contract
reviewed but the PEIA does not conduct them on their own.
Table 1 |
|
| Concern | Benefits |
| Lack of agency wide, consistently applied written procedures for contract administration |
|
| Lack of scheduling information received from Vendors |
|
| No verification procedures when providing TPA's crucial data |
|
| Only one customer satisfaction survey conducted by PEIA in October 1996. |
|
In addition to internal monitoring of contracts, PEIA requires its third party administrators (TPA) to have an independent review (SAS 70's) of their internal controls annually. The term "SAS 70" refers to the American Institute of Certified Public Accountants Statement on Auditing Standard number 70, "Reports on the Processing of Transactions by Service Organizations". These reports are provided following the fiscal year and review the TPA's multiple control procedures in regards to claims processing, rebate processing services, eligibility files, etc. However, the meaningfulness of SAS 70 reviews of contractors' internal controls depends on the effectiveness of PEIA's internal controls. The following passages are qualifying statements from two SAS 70's:
It is the customers responsibility, together with their auditors, to evaluate this information in relation to procedures in place at their organizations in order to assess the total operation of the controls. Further, if effective controls are not in place at the customer location, PCS' controls may not compensate for such weakness.(1)
The relative effectiveness and significance of specific controls at MSBCBC and MMO and their effect on assessments of control risk at the PEIA are dependent on their interaction with controls and other factors present at the PEIA. We have performed no procedures to evaluate the effectiveness of controls at the PEIA.(2)
Based on the above statements from the respective reports, it appears there is much required on the part of the user organization, PEIA. That is, PEIA must have sufficient controls to ensure the service organizations' controls reviewed in the reports are effective.
The passages above are noted because of problems experienced with the PEIA's
eligibility system, the employee information administrative system (EIAS), and the TPA's
systems. Specifically, TPA's claim their information systems have trouble interpreting
EIAS data. This results in inaccuracies in plan membership. Based on our review, the PEIA
did not have a procedure to assure their eligibility information was correct before
submission to the TPA's. The "SAS 70" report performed on the PBM vendor had a
section specifically testing the eligibility controls at the service entity. Within this
section we noted the following which pertains to the PEIA:
User Control Considerations
Users are responsible for ensuring that transactions initiated by the user are
appropriately authorized, complete, and accurate.
Users are responsible for ensuring that output reports received from PCS, are reviewed by appropriate user personnel for completeness and accuracy.
However, the only procedure noted at the PEIA for data accuracy was one in retrospect
when policyholders or billed agency notifies PEIA of errors. In effect this makes the
"SAS 70" less effective because, as the "SAS 70" stated, the controls
in place at the service organization are reliant upon controls within the user's
organization, PEIA. Also, in regards to the SAS 70 audits, it should be noted that these
audits are performed at the end of a fiscal year. The SAS 70's noted above were performed
on TPA's that are no longer contracted with the PEIA, and the reports were submitted to
PEIA subsequent to the expiration of the contracts. Therefore, SAS 70 audit's
effectiveness are contingent upon PEIA's controls and the terms of the contracts being
multiple year. This is not to infer the reports aren't useful for single year plans, just
less effective since modifications implemented due to audit findings would be of no value
to the PEIA.
Specific Examples of Contract Monitoring
As mentioned previously in the methodology section, the Legislative Auditor's Office
reviewed contract monitoring for Pharmacy Benefits Management, Claims Administration,
Utilization Management, and Wellness Services. The following sections are broken down per
service contract type denoting key issues noted during the review.
Pharmacy Benefit Management (PBM)
Merck Medco, Inc. (Merck) Contract - July 1, 2000 to Current
The PBM performs the crucial role of providing prescription drug benefits to PEIA preferred provider benefit plan policyholders. These contracts tend to be of a very complicated nature due to the fact that there are many contingencies involved based on drug ingredient costs, manufacturer rebates and formularies.
Based on our review, it appears the contract for this service is specifically written to allow for specific performance measures to be monitored. Everything from what reports are to be provided and when, claim accuracy rates, response rates to inquiries and customer service telephone average speed of answer. However, what we were unable to observe was how PEIA tracked these.
Merck was awarded the PBM contract based on the PEIA's competitive bidding process as
of July 1, 2000. Due to the short tenure of Merck as the PBM, the scope was limited.
Additionally, the performance standards are based on annual performance. The performance
standards in this contract are broken down in Table 2 below.
Table 2 |
| $25,000 for a Contract Year if Telepaid System Availability Rate averages less than 99.5% for a Contract Year. |
| $25,000 for a Contract Year if Dispensing Accuracy Rate averages less than 99.99% for a Contract Year. |
| $25,000 for a Contract Year if Rx Services fails to meet the dispensing time period standards set forth in Section 5.5 of the Agreement measured on a Contract Year basis. The maximum penalty pursuant to this Section 10.1.3 is $25,000 per Contract Year. |
| $25,000 for a Contract Year if the Maintenance Identification Card Response Rate set forth in Section 5.7 of the Agreement is not met measured on a Contract Year basis. |
| $25,000 for a Contract Year if the direct reimbursement paper claims' response rates of Section 5.11 of the Agreement are not met, measured on a Contract Year basis, subject to a maximum penalty pursuant to this Section 10.1.5 of $25,000 per Contract Year. |
| $25,000 for a Contract Year if the ASA of the customer service telephone line for any Contract Year averages more than thirty seconds measured on a Contract Year basis. |
| $25,000 for a Contract Year if the Telephone Abandonment Rate for a Contract Year averages more than 5% measured on a Contract Year basis. |
| $25,000 for a Contract Year if the Claims Adjudication Accuracy Rate averages less than 98% measured on a Contract Year basis. |
| $25,000 for a Contract Year if the Program Satisfaction Rate set forth in Section 5.13 of the Agreement is not met. |
| $25,000 for a Contract Year if the written correspondence response rates set forth in Sectio 5.9 is not met, measured on a Contract Year basis. The maximum penalty pursuant to this Section 10.1.10 is $25,000 per Contract Year. |
| $25,000 for each of the four most important implementation tasks (as agreed to by PEIA and PAID, in writing) which are not completed by the scheduled completion dates mutually agreed to by PEIA and PAID, in writing, provided PEIA and any applicable third party fully comply with all related implementation requirements, subject to a maximum penalty of $100,000. |
| $250 for each report which is not mailed within the applicable time periods set forth in Section 5.6 of the Agreement, subject to a maximum penalty of $10,000 per Contract Year. |
| $250 for each processable host to host, tape or floppy disc not processed by PAID within the time period set forth in Section 5.8 of the Agreement, subject to a maximum penalty of $10,000 per Contract Year. |
| $25,000 for a Contract Year that the retail pharmacy access guarantee of Section 5.14 is not met. |
For this contract the focus was on the procedures to confirm receipt of information and monitor performance. We obtained the reports submitted by Merck and requested a description of how they were utilized and any supporting documentation. The PEIA had all reports submitted by Merck, but there was no documentation such as schedules showing whether these reports complied with the contract, were timely submitted and within contract parameters. Also, it was unclear how these reports are utilized by the Agency other than they were reviewed for any spikes in data and other specific items. The following items are reviewed by the PEIA monthly upon receipt of reports:
Total drug cost
PEIA paid amount
Member paid amount
Number of claims
Number of members
Amount paid per member
Plan cost share
Member cost share
Single-source, multi source, and generic distribution by claims and dollars
Retail usage
Mail order usage
Retail maintenance network usage
Once reviewed, any concerns are relayed to the PBM. It was disclosed to us that
performance monitoring of the PBM is not a priority at this point since the performance
standards are based on annual performance. However, the Legislative Auditor does not
believe this relieves the PEIA from performance monitoring early in the contract. For
instance, the bolded items within the Table 2 are items in which the PEIA can currently
monitor the vendor's performance. This is especially true since this is a new PBM and
there could be transitional problems that should be noted due to pro-active controls
rather than reactive ones from customer or pharmacy (providers) complaints. Merck Medco
meets regularly with PEIA and also attend the PEIA Finance Board Meetings.
Pharmacy Benefit Management (PBM)
PCS Health Systems, Inc. - February 1, 1999 to June 30, 2000
The PBM First Health, Inc.'s contract was bought out by PEIA for $550,000 in January 1999 with 33 months still remaining on the contract. First Health had been the PBM since 1991. This situation was covered at length by the Legislative Auditor's Office Post-audit Division in its May 21, 1999 PEIA Special Report (See Appendix B). In summary, PEIA bought out the contract because it believed it could save money with another TPA and receive better performance. This led to the contract being awarded to PCS in an "emergency award" since PCS was second in the contract bidding to First Health.
It was noted that the new PCS contract had a savings guarantee. This guarantee was stated as follows:
For the 12 month period beginning February 1, 1999 (the "Guarantee Period"), PCS Health Systems guarantees to the Customer a six million ($6,000,000) savings (the "Guarantee Amount") from the Sixty-eight million dollar ($68,000,000) the Agency projected to spend during the Guarantee Period, based on the Agency's current plan design and level of clinical management, and the assumptions set forth below. PCS will reimburse the Agency for any non-administrative net plan cost, calculated as Customer's total drug spend for the Guarantee Period minus deductibles minus copays minus Customer's Rebate share (the "Drug Spend"), which exceeds sixty-two million dollars ($62,000,000), dollar for dollar not to exceed the Guarantee Amount.
This contract with PCS ended June 30, 2000, yet there is still debate between the PEIA and PCS as to whether this guarantee had been fulfilled. This is due to the fact that the PEIA, subsequent to the initiation of the contract, made changes to the PEIA benefits plan. One change that caused problems was the amount of copays for policyholders. The original guarantee was for a plan with a $40 copay and the change made it a $25 copay. This created a problem because it changed how much was left to be paid by the PEIA affecting the drug spend amount and the guarantee.
PCS is of the opinion that it met the guarantee and the PEIA is of the opinion they did not. PEIA's actuary has made calculations to refute PCS' claims that the guarantee was met. Based on information assembled by the PEIA actuary, PCS still owes PEIA $3,072,586 in guaranteed savings. Per PCS however, it believes it covered the spending guarantee by $3,615,546.
The matters causing debate are due to actuarial adjustments for change in membership and the adjustment for plan changes initiated by PEIA July, September and November of 1999. PEIA has submitted it's actuarial adjustments to PCS to substantiate its claim. As of January 24, 2001, the matter is still being discussed. The guaranteed savings portion of the contract appears to disclose the necessary specifics as to how the reconciliation would be performed. PCS was to provide an estimated reconciliation prior to April 1, 2000 and a final reconciliation prior to September 1, 2000.
During our review of PCS reports there were no performance results reports from the
TPA. This is in light of the contract having specific performance standards by which they
must adhere. Table 3 discloses these below.
Table 3 |
| All Performance Penalties are 10% of Administrative Fees not to exceed 50% of total administrative fees for the plan year. |
| RECAP Help Desk - Telephone inquiries form contracted pharmacies will be answered, on average, in (45) seconds or less. 2% or less of all telephone inquiries will be abandoned. 2% or less of all telephone inquiries will be blocked. |
| PCS Mail Service Shipping - Prescriptions Not Requiring Intervention - 95% of all pharmacist-approved prescriptions requiring no Intervention will be shipped within 2 Business Days. |
| Client Services Administration Calls- Telephone inquiries during Normal Business Hours from customers will be answered on average in 30 seconds. Abandonment rate will be less than 4%. |
| Client Services Administration Implementation - PCS will implement customers on PCS' system as of the effective date of the agreement provided that PCS receives, within the time frames reasonably requested by PCS, complete and accurate implementation information from its customers, including, without limitation, any documents signed by its customers that PCS may reasonably request. |
| Claims Processing - Standard RECAP Processing - 100% of the claims submitted electronically through the RECAP System will be priced in accordance with customers plan guidelines. |
Oddly enough, reporting deficiencies was one reason stated by the PEIA for buying out the previous PBM contract. At any rate, we were however provided with documentation stating that the performance penalty of half the annual administrative fee due PCS would be enforced because of multiple reasons (See Appendix C). This indicates there was some oversight of the TPA's performance, but the method it was accomplished, or determined is not known. Although some items would have been difficult to document, the supporting documentation of these asserted performance problems was not provided. Additionally, the PEIA never made the information available to support these administrative fees were in fact withheld. It is not our position that we do not believe these matters of performance assertions to be true. But, in the event legal action would be necessary against TPA's, we see inadequate documentation being a possible weakness in the States case.
We were able to confirm receipt of formulary rebates from the TPA and trace them to confirm deposit into a State fund. During fiscal year 2000, the PEIA received $2,477,873 in formulary rebates. Formulary rebates are kickbacks from drug manufacturers passed onto the customers by the PBM. It was noted that the PEIA controller tracked these rebates by making estimated receivables based on estimated receivable amounts provided. The PBM made formulary rebate estimates known to the PEIA approximately a quarter of a year prior to the actual payment of the rebate.
Pharmacy Benefit Management Conclusion
The PEIA showed evidence of contract administration such as:
However, there remain control weaknesses and areas for improvement in the PBM contract administration as far as performance monitoring. One cause for this in the opinion of the Legislative Auditor is the multiple responsibilities assigned to one individual. It was disclosed to us by the PEIA that during the 17 month term of the PCS contract, much of the time spent by the individual responsible for contract administration was devoted to developing a request for proposal for the next PBM bid process.
This task left little time for the necessary clerical work to assure the current PBM was performing up to standards. In addition, the work performed by the controller in contract administration is in addition to monthly production of the Agencies financial statements and other essential Agency accounting functions. Thus, the only individuals assigned to PBM contract administration appear to have plenty of duties already assigned which mostly have priority over tasks noted as lacking by this report.
At this time though, it would be highly difficult for the PEIA to efficiently place someone else in the position to handle these tasks. This is because there are no basic guidelines or procedures in which they could follow. The skill set for someone to come in and handle the current contracts without procedures would not be wise cost benefit management.
Additionally, due to the time necessary to develop an RFP subsequent to the emergency award, problems with PCS in lack of reporting and failure to obtain the guaranteed savings, it appears the contract buyout of First Health may not have been a sound decision. Especially since First Health made claims that PEIA's claims against their performance were unfounded. This would have saved the state the buyout money and the transitional problems resulting from the multiple PBM's in the past three years such as data exchange problems. It would also have allowed more time to develop the PBM RFP.
Claims Administration and Management
Mountain State Blue Cross Blue Cross Blue Shield (July 1, 1996-June 30, 2000)
The claims management TPA provides medical claims processing services for the PEIA Plan. The contract for claims management stipulates performance measures for the TPA which are monitored by PEIA. The contract itself addresses that weekly, monthly and quarterly standard reports on the performance quality of the TPA duties are to be delivered from the TPA to PEIA. The content of the reports include such information as interest accumulation to providers, performance standards, physician payments and claims. No consistent and permanent controls are currently in place monitoring claims management TPA's duties.
In July 1996, PEIA contracted Mountain State Blue Cross Blue Shield to provide claims processing and utilization review for the agency. In July 2000, this contract was terminated and Acordia was contracted for claims processing and Intracorp was separately contracted for utilization review.
The contract for claims management TPAs is constructed establishing formulas for penalties and deadlines for reports due to PEIA. These reports and compliance standards from the TPA ensure that performance is accomplished. The agency personnel conclude that the MSBCBS contract was monitored through the contract language itself. However, the contract for MSBCBS does not provide procedural guidelines for PEIA personnel to follow in order to monitor the contract. The contract does not explain contract administration procedures for PEIA staff to maintain penalty controls and checklists for report/financial deadlines.
The MSBCBS contract stated specific performance standards. If these performance
standards were not followed, a penalty was applied to MSBCBS (see Table 4).
Table 4 Penalty Calculations |
|||||
| Performance Measurements | Performance Standards | Rating | Penalty | Rating | Penalty |
| Financially Correct Claims Percentage (Q1) | 98% | 96%-98% | $0.35 | less than 96% | $0.50 |
| Financial Accuracy Percent (Q2) | At least 99.5% | 96%-98% | $0.35 | less than 96% | $0.50 |
| Percent of Claims Finalized in 12 Working Days (T1) | At least 92% | $0.50 | |||
| Telephone Calls Abandonment Percentage (A1) | 2% or less | $0.25 | |||
| Average Speed of Answer in Seconds (S1) | 30 seconds or less | $0.25 | |||
| Blockage Percentage on Calls (B1) | 1% or less | $0.25 |
*Penalty amount is determined by multiplying the average number of members during the quarter by the rates described above.
If these performance standards were not met monthly, MSBCBS provided a penalty amount to PEIA which was deducted out of the administrative costs. For example, compliance reports and invoices indicate that for the months of April and May 1998 penalties totaling $15,418 were deducted from FY 1999 administrative expenses to MSBCBS for inadequate TPA performance of T1 (Timeliness Standard) and Q2 (Financial Accuracy Amount). The administration of these penalties included the manager of the MSBCBS contract sending correspondence to MSBCBS informing them of the penalty, a copy of which was sent to the PEIA finance entity to alert them of reduction in administration expenses for MSBCBS. PEIA was not able to provide the Legislative Auditor with FY 2000 penalty invoices. Moreover, there were no consistently applied checks in place to establish that these penalties were enforced and no communication between the financial entity of PEIA to the MSBCBS contract manger to confirm that financial penalties are enforced. With no written procedures in place describing how to monitor the penalty process or to ensure performance standards, there remains the possibility that MSBCBS was not charged correctly or at all for penalties. The lack of organization and controls over performance standards left PEIA with the possibility of MSBCBS providing poor performance without MSBCBS being penalized.
In December 1998, PEIA amended the contract with MSBCBS concerning penalties. The contract was amended to include incentives for MSBCBS on performance standards. This included the same performance standards that were set forth for penalties including Q1, Q2, T1, A1, S1 and B1. It was determined that PEIA would pay MSBCBS quarterly incentives for fulfilling these standards, whereas MSBCBS would pay PEIA quarterly penalties for not accomplishing the performance standards. This amendment is puzzling because MSBCBS should be doing its contracted performance of the contract to fulfill the contract and accept its end of the agreement for which they are being paid to do. The concept that MSBCBS was rewarded further through an incentive in the contract for a standard they should have done through the contract itself appears to be flawed. Invoices obtained by the Legislative Auditor show that for FY 2000 PEIA paid MSBCBS $336,724.73 in incentives. The PEIA did not provide invoices or evidence to prove whether or not the penalties inflicted on MSBCBS lesson or equaled the amount of incentives paid back to MSBCBS because PEIA cannot account for penalties charges to MSBCBS for FY 2000. The incentive performance standard provision was eliminated when Acordia was contracted in July 2000.
It is important to note that the contract manager for this contract has kept all performance standard reports from MSBCBS up to FY 1999 and provides spreadsheets to evaluate and document their performance. This system of contract documentation is developed and catered by the contract manager. This method works efficiently when the contract manager is present. However, at the time of this review, the contract manager was on leave. Because no written procedures exist on how to monitor the contract, the PEIA staff was at a loss to find contract documentation, reports and operational controls after FY 1999 for the contract. The staff was also unable to locate or provide information on performance standards for S1 (Speed of Answer) and B1 (Blockage Percentage on Calls). This individualization of contract controls leaves the agency in a position of vulnerability if the contract administrator absents the position.
MSBCBS was responsible for providing reports other than performance standards. The PEIA
filed these reports. Examples include MSBCBS interest reports documenting interest paid to
providers from MSBCBS after the 65 day claim period and MSBCBS/PEIA operations weekly
inventory reports detailing days payable for claims and billed charges. Utilization
review, another contracted duty of MSBCBS was reviewed for performance by PEIA through
MSBCBS Utilization Management Reports. These reports were filed and received by PEIA in
accordance with the contract. However, there is no documentation showing how these reports
were utilized by PEIA. The PEIA does not show documentation of whether the reports were
submitted within timeliness or standard parameters set in the contract.
Acordia National, Inc. (July 1, 2000-present)
The PEIA awarded Acordia the claims management through the competitive bidding process
effective July 1, 2000. The contract for Acordia is similar to the MSBCBS contract with
the exception of utilization management. Due to the short period in which PEIA has
obtained Acordia as the claims management TPA the scope was limited. The focus on the
Acordia contract is limited to the monitoring procedures for transition between claims
management TPAs.
The PEIA alleges that due to the transition between contracted TPAs, PEIA has not received reports necessary to review Acordia's performance to date. The explanation given by PEIA for lack of reporting is that Acordia has given most of their resources and staffing to deal with claims backlog. The PEIA has not received the reports data in order to evaluate Acordia's performance or apply penalties. (See Table 4 for performance and penalty standards.) This situation is being handled between Acordia and PEIA through weekly meetings to discuss claims backlog, customer service issues and reporting status from Acordia to PEIA. Acordia currently produces their monthly procedure claim reports and phone statistics for customer service. This appears to be the only documented monitoring procedures in place implemented by PEIA to manage the transition period.
There is evidence that PEIA has not been satisfied with Acordia's performance. The former director of the PEIA issued a letter to Acordia in November 27, 2000 providing notice that if Acordia did not resolve compliance issues set in the contract within sixty days then action would be taken to protect the insureds of this program and taxpayers of the state of West Virginia. This notice outlined a number of concerns over Acordia's performance including unacceptable claims backlog, no establishment of acceptable Eastern panhandle out-of-state network and member confusion over network providers. The PEIA was not able to provide the Legislative Auditor documentation confirming that Acordia is not meeting these requirements. The Acordia contract may be monitored retroactively through consumer complaints brought to PEIAs customer service. This is a plausible conclusion to make since there is no documentation of Acordia's performance. The monitoring of Acordia does not appear to be established pro-actively but rather in a reactive manner. It should be considered that PEIA come up with procedures to monitor and enforce the Acordia contract in order to provide performance standards, savings and quality due to PEIA when Acordia does not reach their contract requirements.
Wellness Program Contract
The PEIA is charged with the responsibility of providing a wellness program per
§5-16-8(9) of the West Virginia Code. The wellness program is required to include plan
incentives to discourage tobacco use, alcohol and chemical abuse and an educational
program to encourage proper diet. This section also requires the PEIA to contract with
county boards of education for the use of facilities, equipment or any service related to
the wellness program. It was noted the PEIA had not contracted with any county boards of
education for facility use. The PEIA received a glowing accommodation for its innovative
program. This came in the way of an article in Business & Health (See Appendix
C). The program is known as "Pathways to Wellness".
Partners in Corporate Health - July 1, 1997 to Current
PEIA contracted with Partners in Corporate Health to administer the wellness program. We
obtained reports submitted by Partners in Corporate Health (PCH) that outline the
accomplishments, goals, and effectiveness of the program. The Pathways website was also
visited and all but two links on the site were functional and therefore operating
effectively. PCH provides quarterly reports complete with handouts given at worksite
activities, examples of the newsletters sent to the PEIA policyholders homes, various
flyers, newsletters and brochures for various programs. These are kept on hand at the PEIA
and the president meets with the PEIA weekly and makes presentations to the PEIA Finance
Board on the programs accomplishments.
The Pathways to Wellness program provides a website, worksite activities such as health screenings, blood pressure screenings and other health promoting activities. The program conducts satisfaction surveys, compiles membership claim data and vital statistics. This information is then used to produce return on investment data to help evaluate the effectiveness of the program. It is also helpful in determining the average claim cost for low risk vs. high risk members. It was noted during the review of reports that PCH reported during Phase III the Pathways project was honored with the "Exemplary Public Worksite Wellness Program" Award by the National Association of Public Worksite Health Promotion.
The evolution of the PEIA wellness program has went through four phases since its inception in 1992. Phase IV was recently completed and although the final evaluation report hasn't been completed, PCH disclosed that there are now over 126 worksites as of January 2001 and over 10,000 enrolled. The worksites will soon total 230 in Phase V.
The program has also implemented a smokers cessation program that over it's time has had 3,590 medicaid enrollees and 827 PEIA enrollees. There is a telephone number that policyholders can reach the Pathways smokers cessation program by dialing 1-877-Y NOT-QUIT. The program also tabulates any prescriptions issued to aid in quitting. As of September 2000 the formal evaluation for the YNOTQUIT program had just begun. As of December 2000, the Quarterly Report had no mention of evaluation results for the smokers cessation program.
Wellness Contract Conclusion
The program is highly capable of producing numbers showing the programs activity,
productivity and effectiveness. The Legislative Auditor inquired with the PEIA as to what
procedures were in place to oversee this program and validate the program's figures in
effectiveness. We also interviewed with a representative of PCH to gain further
understanding of the evaluation process of the program. Outside of the reports submitted
and the regular meetings it was disclosed to us there were no other means of verifying
validity.
However, all reports submitted do include an example of an actual sign in sheet of an activity performed at worksites and an example of a survey form which had been performed, etc. So there is some proof of activities submitted in reports. The Legislative Auditor requested examples of source documents such as sign in sheets for activities and smoker cessation enrollment directly from PCH. PCH obliged our request and submitted these documents without delay along with explanations as to how they arrive at their ROI numbers. This is one method that takes little time to perform and is effective in making sample confirmations as to activity number verification.
The PEIA's smoker cessation program cost share for the 2000 program that extends to June 30, 2001 estimated costs total $203,473. The current Phase IV program for January 1, 2000 to June 30, 2001 will cost the State $977,922 in fixed cost and there will variable costs in addition to this based on activities performed by PCH not to exceed $190,000. In the event the Pathways program reaches the maximum allowable variable costing, there will be a total of $1,371,395 spent on these programs. Based on these budgeted cost figures, it appears validation procedures would be warranted.
Utilization Management Contracts
Utilization management is a crucial aspect of claims processing. This is the step in which
certain medical procedures are scrutinized prior to application to determine the necessity
and if this is the best procedure to perform. Medical care providers are given a list of
procedures or situations that require prior review before it can be administered and
honored by the PEIA. This process is known as pre-certification. Utilization management is
a cost saving measure based on reducing unnecessary utilization of plan benefits. A
segment of the section titled Duties of Intracorp in the contract states:
In exercising its responsibilities under this Agreement, Intracorp shall use its best efforts to assure that health care is provided to insureds with the least costly combination of services which are actually medically necessary without compromising or diminishing the quality of the health care or outcomes resulting from the health care delivered to the insureds.
Intracorp - July 1, 2000 to current
Intracorp was awarded the utilization management through the competitive bidding process as of July 1, 2000. The contract has specific performance measures, services and what reports are to be provided. In providing its service to the PEIA Intracorp utilizes licensed, board certified or eligible physicians, psychologists and counselors with graduate degrees in their specialties, and registered nurses employed or engaged by Intracorp. Intracorp performs its services in compliance with the PEIA plan document which is an attachment to the contract.
Based on our review, all reports were provided as dictated by the contract. The reports denoted any cost saving incurred by the PEIA due to utilization management. All performance reports were also provided.
It was disclosed to us verbally that the PEIA utilizes these reports by monitoring the percentage of approval for reviewed procedures. If, for example, a certain procedure is approved 100% of the time there is no need to continue reviewing this procedure. But, we weren't sure of this procedure's purpose since the current contract's billing is based on the number of eligible members and not per utilization review.
As with other contracts handled by the PEIA, Intracorp meets frequently with the PEIA staff. These meetings also include representatives of Acordia. This is due to the fact that there is a necessary relationship between the two entities. It is necessary for Acordia to sometimes wait for Intracorp's approval before some claims can be paid by Acordia. Since all current contracts were issued on the same day, July 1, 2000, there have many transitional problems occurring. It was noted that Acordia notes one of its reasons for high claim backlogs is due to the required interaction with Intracorp.
Mountain State BlueCross and BlueShield (MSBCBS) - July 1, 1996 to
June 30, 2000
MSBCBS handled utilization review along with claims administration. We were able to obtain
utilization reports for the period of July 1997 to December 1999. These reports were much
more limited than the current utilization management vendor but did break down savings for
the PEIA. The PEIA had a plan compliance review performed on MSBCBS for the period of
January 1, 1998 to June 30, 1999.
One item focused on during this review was the utilization pre-certification process
and other utilization processes performed by MSBCBS. This review noted exceptions in this
process. For example, the review noted 16 claims submitted for claims processing were
assigned a different diagnosis related group (DRG) category by the MSBCBS CAPS claims
processing system than the DRG category assigned by the MSBCBS pre-certification system.
The reviewing auditor's concern regarding this matter was that there was not a procedure
in place during the precertification process to confirm the discharge DRG and communicate
to the claims processors the appropriate DRG category to utilize during payment.
Basically, the reviewing auditor's had concern regarding the effectiveness of the MSBCBS's
utilization review.
Utilization Management Conclusion
Based on our review of the utilization management contract administration, the PEIA used an independent review of the utilization management vendor to monitor performance. This review was effective in helping determine that there were issues regarding the utilization management performed by MSBCBS and acted accordingly. MSBCBS did not specialize in this function and the PEIA now retains the services of a vendor that does in fact specializes in this field. Hopefully PEIA will in fact save the state money by making this move.
Internally however, the PEIA does not appear to have procedures for monitoring utilization management vendors other than the retention of reports submitted by the vendor. Utilization management is a crucial cost saving tool which could be used to help develop future cost efficient insurance plans if data received is utilized. Also, there were no procedures to verify all reports were received, timely and in accordance with the contracts.
Recommendation 1:
The PEIA should develop written procedures to monitor the performance of it's TPA's.
Recommendation 2:
The PEIA should reallocate personnel resources within the current PEIA staff to assist
current personnel assigned contract administration. The position would assure all required
data is received, performance standards met and maintain contact with finance and benefits
administration personnel.
Recommendation 3:
The PEIA should develop procedures to ensure proper data transmissions with TPA's.
1. PCS Health Systems, Service Auditor's Report Claims and Rebate Processing Review for the period July 1, 1999 to June 30, 2000
2. Mountain State Blue Cross Blue Shield, PEIA Claims Processing System, Report on Controls Placed in Operation and Tests of Operating Effectiveness, for the period May 1, 1999 to April 30, 2000.